Hospitals, Insurance Firms Can’t Deny Cashless Claims For Covid Patients; Govt May Take Action Against Them
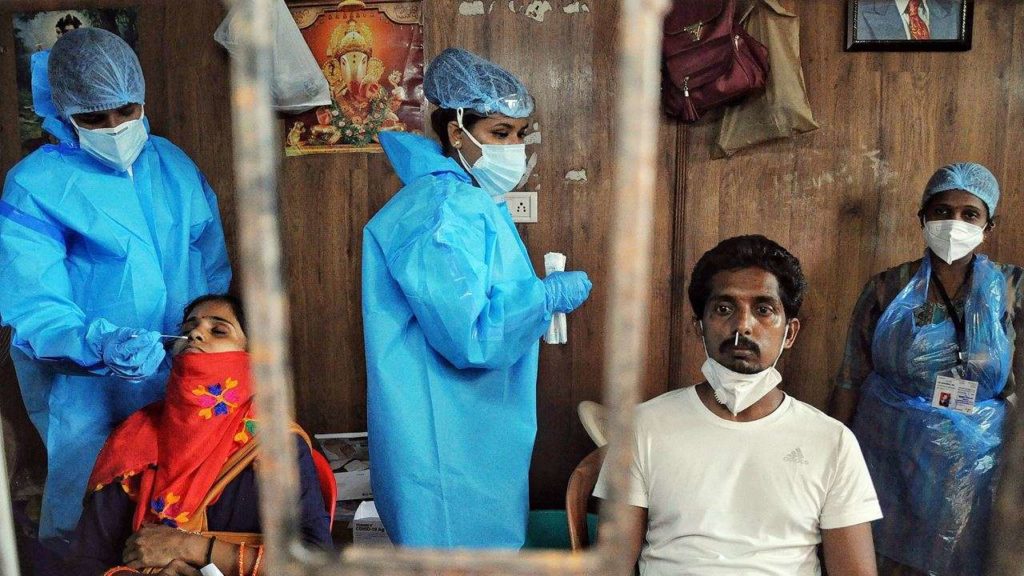
Reports of hospitals denying cashless insurance facilities for treatment of Covid-19 positive patients (policyholders) are taking rounds in the media.
Addressing this issue, Finance Minister Nirmala Sitharaman spoke to the regulatory body, IRDAI chairman Subhash Chandra Khuntia on Thursday, and directed him to take immediate action upon such complaints by insurance companies.
In response to the FM’s addressal on the matter, Khuntia asked all the insurers to expedite the process of finalised settlement claims of COVID-19 treatment, on Friday.
Sitharaman Mandates Hospitals to Abide T&C of SLA
On Thursday, Sitharaman asked IRDAI chairman to address all the complaints regarding denials of cashless claims by insurance companies.
She informed many hospitals, reportedly are denying cashless facilities for treating Covid-19 patients, when these policyholders are entitled for the cashless treatment under their policy.
She affirmed that hospitals which are in arrangement with insurers for providing cashless facilities are obligated to provide cashless treatment for all treatments, including the Covid-19 ones.
The Finance Ministry stated, “All the Network Providers (hospitals) who have signed Service Level Agreements (SLA) with general and health insurers have to mandatorily provide cashless facility for any treatment to the policyholders including Covid-19 treatment in accordance with agreed provisions of SLA and terms and conditions of policy contract.”
The ministry adds that if a cashless facility at any such enlisted hospital(s) is denied, the policyholders are free to lodge a complaint against such an entity to the concerned insurance company.
Sitharaman informed via tweets that she spoke to Chairman, IRDAI Shri SC Khuntia to act immediately, in response to these complaints.
IRDAI Asks Insurers to Conduct Immediate Settlements
After meeting with FM Sitharaman on Thursday, Khuntia asked insurers to expedite the process of settling claims on a cashless basis for Covid-19 treatment.
It also asked hospitals to not differentiate patients, in regards to admission or treatment.
Addressing the issue of cashless claims being denied to Covid treatment policyholders, the regulator stated in a circular,
“In compliance with the provisions, the insurers, in case of ‘cashless claim’ under a health insurance policy, are advised to ensure expeditious settlement of such claims on a cashless basis in accordance to the Service Level Agreements (SLAs) entered with hospitals.”
“All hospitals are also requested not to differentiate the patients in terms of admission or treatment whether they are insured or not insured or whether they pay cash or avail of a cashless facility.”, it added.
The regulator also asked insurers to ensure that policyholders are charged as per the rates agreed to by network providers wherever applicable.
Further, all insurers have been directed to ensure that the “reimbursement claims” under a health insurance policy should be settled expeditiously, states Business Today.

Comments are closed, but trackbacks and pingbacks are open.